
If cancer cells are not found, no further surgery is necessary. Other cancers may include: Non-small cell lung cancer. The sentinel node biopsy is commonly used for patients with melanoma and breast cancer. Sentinel nodes harvested by dual technique, if found negative on intraoperative frozen section, can prevent breast cancer patient from a potentially debilitating complete axillary clearance. A pathologist then views the tissue under a microscope to look for cancer cells and often uses additional tissue stains (immunostains) to determine whether microscopic evidence of melanoma is evident in the regional lymph nodes. The sentinel lymph node biopsy is necessary for patients with possible cancer to deduct a spread into the lymphatic system. Aim: The long term safety of sentinel lymph node (SLN) biopsy during pregnancy is insufficiently explored, mainly due to fear for fetal safety. This first lymph node(s) to receive the tracer is removed for biopsy. A body scan is then performed to help the surgeon localize the sentinel lymph node before beginning the operation. The injection of the radioactive tracer is performed in the Nuclear Medicine Department either the evening before surgery or several hours before surgery. The radioactive tracer or dye flows through the lymph channels in the skin to first draining lymph nodes in the region(s) around the melanoma. A radioactive tracer and/or blue dye is injected near the tumor before surgery in a process called lymphatic mapping (or lymphoscintigraphy). Most patients resume regular activities within a few days and incisions generally heal within a few weeks.The removal of the sentinel lymph node (the first lymph node to which the cancer is likely to spread). 
easier for the patient in terms of recuperation.A negative sentinel lymph node indicates a greater than 95 percent chance that the remaining lymph nodes are also cancer-free more accurate than the traditional axillary dissection in assessing whether breast cancer has spread to the lymph nodes.highly reliable in detecting cancerous cells A sentinel lymph node is a node or nodes that is likely to be the closest node draining a cancer, making it the earliest to show if a metastasis has occurred. 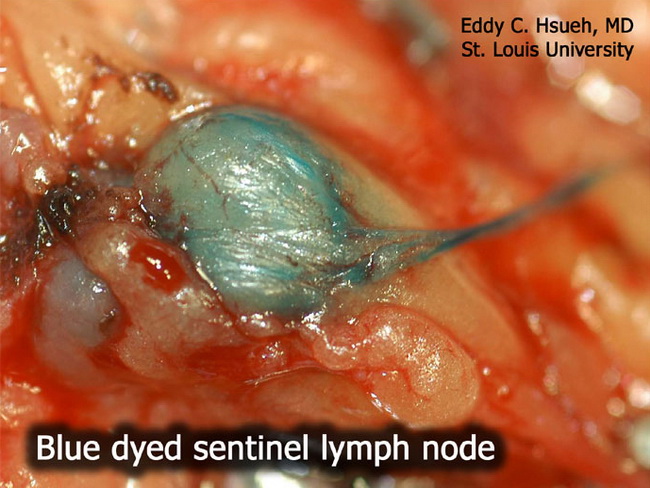
In less than five percent of sentinel node biopsies, the sentinel node cannot be identified and a full axillary dissection is done. Only the lymph nodes that have absorbed the radiotracer are removed. The surgeon makes an incision underneath the arm and passes a hand-held probe over the area to measure levels of radioactivity. Images may be taken to help the surgeon visualize the radiotracer’s ’s pathway as it leaves the breast. Prior to surgery to remove part of or the entire breast, a tiny amount of radioactive particles are injected in the area of the breast where the tumor is or around the nipple. In a sentinel node biopsy, only the sentinel nodes are surgically removed, which results in fewer complications and side effects for the patient, including lymphedema. Sentinel nodes collect the fluid draining from the tumor and are most likely to contain cancer cells if the tumor has metastasized, or spread. Molecular imaging is used to identify the first few, or sentinel, nodes into which a tumor drains. The procedure is performed in the operating room under. Your surgeon will explain the timing of the procedure and what preparation is required. It is sometimes performed as a separate procedure. A sentinel node biopsy is an established alternative to axillary lymph node dissection. Sentinel node biopsy, also termed sentinel node dissection, is usually performed at the time of your breast surgery, either lumpectomy or mastectomy.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
